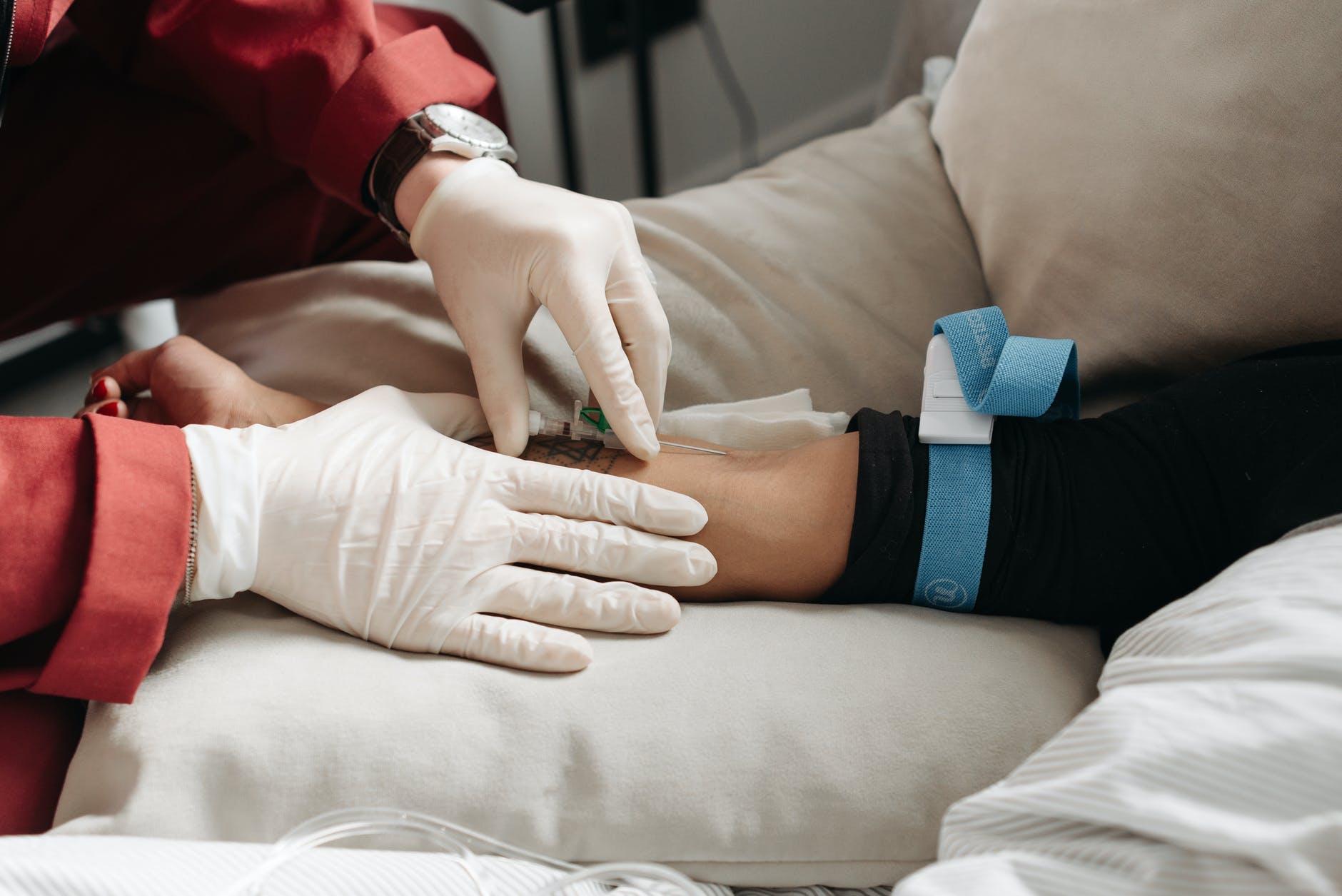
What is jaundice?
Jaundice is the yellow discoloration that can be seen in the skin and the sclera of the eyes when there is an accumulation of bilirubin in tissue.
Bilirubin is a chemical that is formed from the removal and breakdown of old red cells by the reticuloendothelial system.
Hemoglobin in red cells is broken down and the iron in the haem groups are reused by the body while the porphyrin ring is degraded into bilirubin.
Bilirubin metabolism
There are two types of bilirubin: conjugated, and unconjugated.
conjugation simply refers to the addition of charged substances to a molecule, so it can become soluble.
Bilirubin is insoluble in its unconjugated form. Unconjugated bilirubin needs to be sent to the liver to become conjugated.
Unconjugated bilirubin is transported in the bloodstream bound to albumin and is then taken up by liver hepatocytes and sent to the smooth endoplasmic reticulum where it undergoes conjugation with glucuronic acid.
This reaction is catalyzed by the enzyme UDP-glucoronyltransferase.
Conjugated bilirubin (which is now soluble) is added to bile and secreted into bile canaliculi and eventually reaches the small intestine.
In the small intestine, bilirubin is converted into urobilinogen by gut bacteria.
This compound is then oxidized to stercobilin, which is the brown pigment that gives feces its characteristic color.
Diseases, disorders, and laboratory testing
1. Gilbert’s syndrome
Gilbert’s syndrome is the most common inherited cause of unconjugated hyperbilirubinemia.
Unconjugated hyperbilirubinemia refers to increased levels of unconjugated bilirubin.
It is a familial autosomal dominant trait caused by the decreased expression of UDP – glucoronyl transferase which is the enzyme involved in conjugation of bilirubin with glucuronic acid.
Unconjugated hyperbilirubinemia is usually asymptomatic.
There is no bilirubinuria (which is bilirubin in urine) and most patients have a plasma level less than 50micromol/l.
mild hyperbilirubinemia can also be seen in patients with hemolytic anemia.
Hemolytic anemia is caused by the abnormal breakdown of red blood cells at a rate quicker than they can be supplied from bone marrow.
Hemolytic anemia and gilberts syndrome can be differentiated (as they both show hyperbilirubinemia) using a full blood count (FBC) where reticulocyte count (immature red blood cell count) will be normal in gilberts syndrome and increased in hemolytic anemia.
This is because the body tries to keep up with the increased demand for RBC’s by increasing the production of new cells, increasing the amount of immature red blood cells circulating.
A confirmatory test for gilberts syndrome is monitoring plasma bilirubin in a state of reduced energy for 72 hours.
This can be done by restricting the patient’s daily caloric intake to 300kcal. In patients with GS, there is at least a doubling of unconjugated plasma bilirubin levels whereas normal individuals won’t rise above 25 micromoles/l.
2. Cholestasis
Cholestasis refers to blockage of bile ducts which results in reduced flow of bile (and therefore bilirubin) into the small intestine.
Cholestasis can be caused by problems outside the liver (extrahepatic) such as blockages due to gallstones.
Tumors and certain drugs can cause intrahepatic obstructions.
Since this disorder isn’t due to reduced liver function, the major form of bilirubin that accumulates is the conjugated form as the liver has already performed conjugation with glucuronic acid.
In cholestasis urobilinogen often becomes undetectable in urine which is abnormal.
The patient’s stool is often pale due to a lack of stercobilin pigment (which is the brown pigment responsible for giving feces color) being formed in the gut.
Plasma tests will often show ALP and GGT (which are proteins commonly found in the liver) levels rise to 3 times the upper reference limit.
There is also a moderate rise in ALT and AST activity (which are also proteins commonly found in the liver).
3. Cirrhosis
Cirrhosis is another disorder that can lead to jaundice. Cirrhosis can occur when there is repeated death and regeneration of liver cells leading to fibrosis and scarring.
Causes include chronic excessive alcohol intake and autoimmune diseases such as autoimmune hepatitis.
In mild cirrhosis, no clinical abnormalities may be apparent until later in the disease.
This is because the liver has great functional capacity meaning it would have to be damaged extensively to produce symptoms.
The ratio of AST to ALT can be used as a test for cirrhosis. Values greater than 1 provide good sensitivity and specificity for diagnosis.
4. Hepatitis
Hepatitis is the inflammation of the liver, caused by hepatitis viruses as well as the Epstein-Barr virus.
Hepatitis can also be because of ethanol and paracetamol abuse, as well as due to autoimmune problems.
Viral hepatitis very commonly causes acute (quick onset) liver cell damage which leads to reduced liver function and therefore jaundice.
Blood tests will reveal a rise in total bilirubin (which will be mostly unconjugated) as the decreased liver function will reduce the rate of bilirubin metabolism.
Blood tests will also show a rise in AST and ALT levels. If the damage to the liver begins to cause intrahepatic biliary obstruction, ALP and GGT levels may begin to rise as a result.
Summary
- Jaundice is a yellow discoloration of the skin caused by increased bilirubin concentration in tissue.
- Damage to the liver and or blockage to bile ducts can cause jaundice. Jaundice can also be caused by hemolytic anemia.
- If the damage is to the liver, there will be a rise in total bilirubin, most of which will be unconjugated. there will also be rises in AST and ALT levels.
- If jaundice is due to cholestasis, there will be a rise in total bilirubin, most of which will be conjugated. There will also be a rise in ALP and GGT levels.
- The blockage of bile ducts also causes low levels of urobilinogen in urine as well as a pale stool.
- The liver has a great functional capacity, so it would have to be damaged quite extensively to show symptoms of a disease.
![[MacOS Error] – Compressor does not support running in a macos virtual machine](https://cdn-0.ghoopi.com/wp-content/uploads/2023/09/img_6688-150x150.jpg)